U.S. Taxpayer Funded Initiative Trains Dentists to Push HPV Vaccine
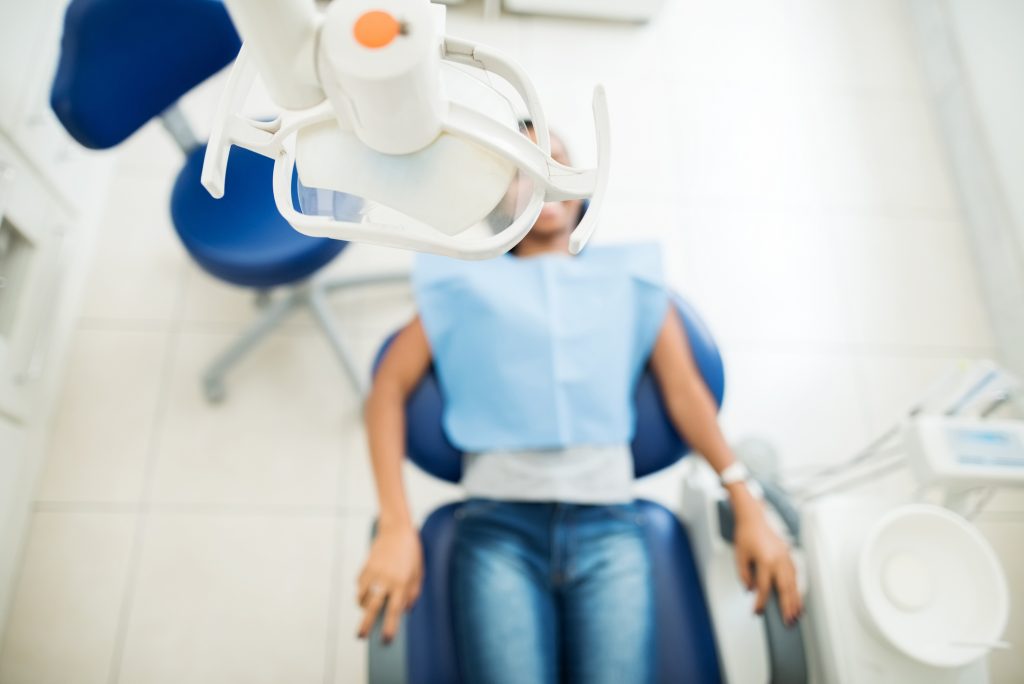
In recent years, government health agencies, cancer societies, as well as the American Dental Association (ADA), have attempted to recruit dentists to advocate for patients to get the human papillomavirus (HPV) vaccine to prevent oral cancers. An HPV Vaccine Roundtable initiative, funded largely by the U.S. Centers for Disease Control and Prevention (CDC), advises dentists […]
Pediatricians Get Paid to Push Vaccines. And It’s No Small Amount of Cash.

Opinion | In April 2023, I reported how primary care providers across the U.S. were bribed with incentive programs to coerce patients into getting the toxic COVID-19 shot. Since there was no medical malpractice liability, doctors profited while patients risked their lives as participants in an unprecedented medical experiment, all while being lied to about […]
Health Care Staff Shortages a “National Emergency”
Hospitals and other health care facilities in the United States are suffering a workforce shortage, a crisis that was brewing before the COVID-19 pandemic but has only been amplified since then. The American Hospital Association (AHA) calls the shortages a “national emergency” and, although it is most acute in the nursing field, the effects are […]
Big Pharma’s Influence on U.S. Medical Schools is Significant

An informal survey of medical schools conducted in 2005 by National Public Radio (NPR) showed that a number of universities and academic institutions are funded by pharmaceutical giants and other health industry sources. The survey, carried out through telephone calls and internet searches, found that two to six percent of the yearly budget of medical […]
Gallup Poll: More Americans Dissatisfied With Quality of Health Care

A recently released Gallup poll revealed that, for the first time in 20 years, less than half of all Americans are very satisfied with the quality of the health care system in the United States. The poll indicated that only 48 percent of Americans rated the quality of the health care system as “excellent”—a notable […]
Study Finds 25 Percent of Hospitalizations Result in Health Care Related Injuries

A new study published in the New England Journal of Medicine found that hospital related adverse events were identified in nearly one in four hospital admissions, and that approximately one in four of the events were preventable.1 “The authors’ findings are disturbing. These findings suggest that the safety movement has, at best, stalled,” said Donald […]

