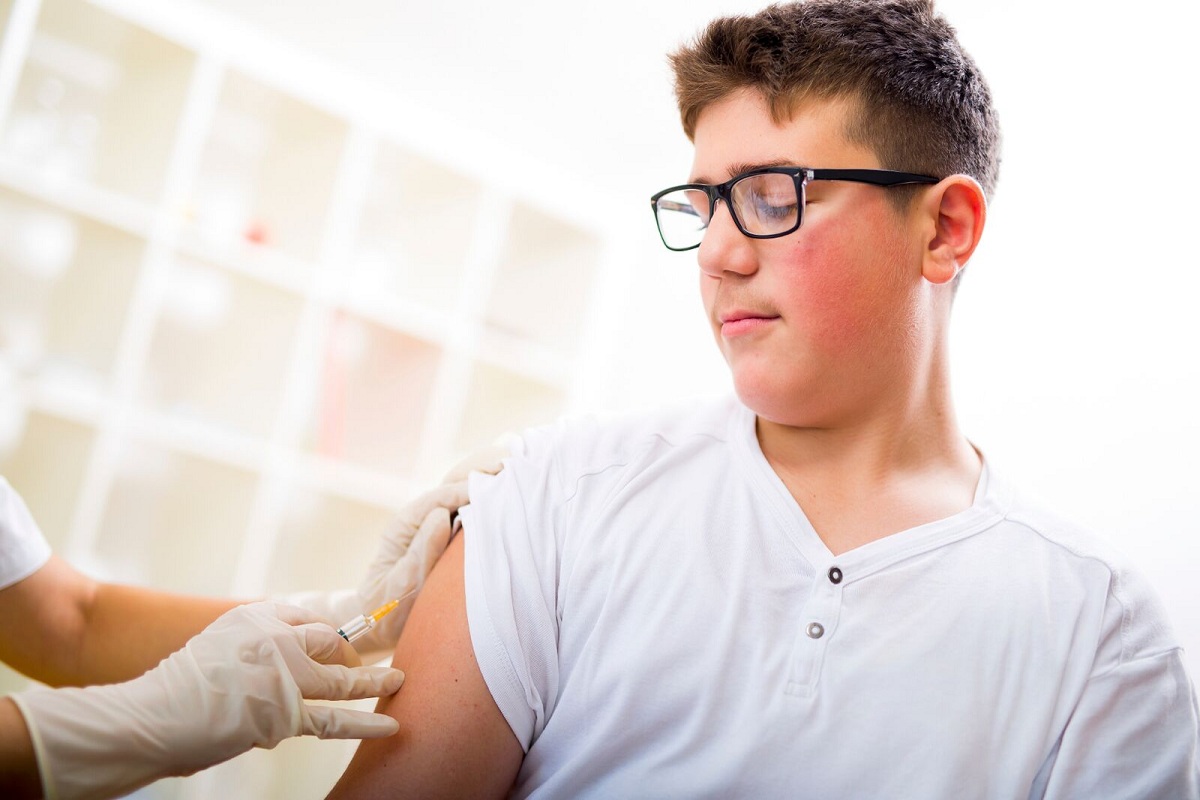
There has been an increase in the numbers of reported cases of B. pertussis (whooping cough) in the United States in recent decades, especially in the past few years. Reported outbreaks of the highly contagious disease have commonly been attributed to waning protection of the pertussis vaccine and low vaccine coverage.
Additionally, researchers have been arguing about whether the B. pertussis organism started evolving shortly after the whole cell DPT vaccine was given on a mass basis to children in the late 1940s followed by introduction of less reactive acellular DTaP vaccine in the mid 1990s.1 However, now there is wider recognition of scientific evidence that data in recent years points to a fourth cause—asymptomatic transmission of whooping cough by vaccinated individuals.
Reported Whooping Cough Cases Increasing for Decades
In 1922, there were 107,473 reported cases of pertussis in the United States and 5,099 deaths.2 Pertussis-related mortality declined during the 1940s largely due to improved sanitation, hygiene and access to health care. Although there was a general decline in reported pertussis cases after the DPT vaccine was introduced in the late 1940s, reported cases began to increase in the 1980s.3 One 1977 study published by the U.S. Centers for Disease Control and Prevention (CDC) found whole cell DPT vaccine effectiveness was only 63 percent.4
There were 1,010 reported cases of pertussis in the U.S. in 1976 and 25,827 cases in 2004, for a nationwide incidence of 8.5 pertussis cases per 100,000 individuals.5 However, by 2012, there were approximately 48,277 cases of pertussis reported in the U.S.6
Waning Vaccine Effectiveness Faulted for Pertussis Outbreaks
Currently, there are three hypotheses being publicly discussed to explain the reported resurgence of pertussis in the highly vaccinated U.S. population: (1) suboptimal vaccination rates; (2) waning immunity of vaccinated individuals; and (3) evolution of the B. pertussis organism to evade vaccines. The first hypothesis—suboptimal vaccination rates—is not supportable because the U.S. has had a 95 to 98 percent vaccination rate among kindergarten children for the past three decades.7 8
In the U.S., the pertussis vaccine is administered in a combination shot that contains vaccines for diphtheria (D), tetanus (T) and pertussis (P). Due to frequent serious complications, including brain inflammation and permanent brain damage, the older whole cell pertussis vaccine (DPT) that was created in the early 20th century was replaced in 1996 by a purified, less reactive acellular vaccine (DTaP). Although whole cell DPT vaccine is still used in parts of Africa, Asia and the Middle East, children in the U.S., Europe and most other developed countries other countries receive four to five doses of acellular pertussis DTaP vaccine by age six and a booster dose of Tdap vaccine in their adolescent years.9
Evidence suggests that the temporary natural immunity provided by B. pertussis infection and the temporary immunity provided by pertussis vaccines play a role in reported outbreaks of whooping cough.
A 2005 case-control study estimated the effectiveness of DTP and DTaP vaccines to range from 83.6 percent to 97.7 percent, depending on the number of doses administered, vaccine combinations used and age of the child at administration.10
A 2012 analysis of a pertussis outbreak in California revealed that pertussis vaccine effectiveness was 41 percent for children aged two years to seven years, 24 percent for children aged eight years to 12 years and 79 percent among adolescents aged 13 years to 18 years.11 A second 2012 study examining the 2010 pertussis outbreak in California confirmed waning protection from the five-dose DTaP series each year after the final dose.12
A 2013 study backed up these findings by evaluating the protection of the five-dose DTaP series for children born between 1998 and 2003 in Minnesota and Oregon. The incidence of pertussis for the fully vaccinated children rose each year following the fifth dose of the vaccine.13
The CDC issued a press release about the 2012 pertussis outbreak in Washington state acknowledging that pertussis vaccine immunity begins to wane within five years. CDC officials also stated that unvaccinated individuals and children with vaccine exemptions are not responsible for reported whooping cough outbreaks.14
In fact, 73 percent of the children aged seven years to 10 years and 81 percent of the adolescents in Washington with pertussis infections had been fully vaccinated.15
Vaccine Failure Again to Blame
While the evidence for waning vaccine immunity over time has received considerable media attention, relatively few people know that vaccinated persons can become infected and transmit pertussis to others without showing any symptoms.
In a 2014 study, FDA researchers found that non-human primates vaccinated with both whole cell and acellular pertussis vaccines were often protected from severe symptomatic disease but could still become infected and transmit pertussis to close contacts. Although the infant baboons who had received whole cell pertussis vaccine in the study more rapidly cleared the infection and, therefore, transmitted pertussis for a shorter period of time, the baboons given acellular pertussis vaccine also became infected and asymptomatically transmitted disease to close contacts.16
Given this biologically plausible explanation for reported resurgence of pertussis in highly vaccinated human populations, two researchers from Santa Fe Institute, a nonprofit research center, collected empirical data from the CDC on reported pertussis cases in the U.S. from 1922 to 2012. Because of a similar rise in reported cases of pertussis during the past 20 years in the United Kingdom, the New Mexico researchers also collected data on pertussis cases reported in England from 1940 to 2013. These periods accounted for a time when there was no pertussis vaccination and times when whole-cell and acellular pertussis vaccines were used. Coupled with genomic data, the investigators created a detailed epidemiological model of whooping cough transmission.
Their conclusion, which they published in 2015, was that vaccinated individuals may not display any symptoms of whooping cough, but can still be infected with the bacterium and unknowingly spread the disease multiple times in their lifetime. This asymptomatic transmission not only contributed to the observed increase in pertussis incidence over the years, but may have exacerbated it.
Further, the model showed that vaccinating parents, siblings and other individuals in close contact with unvaccinated infants too young to receive pertussis vaccine—a theoretical method of protection that public health officials call “cocooning” may be completely ineffective. The researchers also pointed out that the theory of achieving “herd immunity,” which is supposed to be accomplished when a high enough proportion of individuals in a population have been vaccinated in order to protect unvaccinated individuals, was also impractical for pertussis vaccine according to the model.
“Clearly, more research is necessary, but if our results hold, public health authorities may be facing a situation similar to that of polio, where vaccinated individuals can still transmit infection,” the researchers wrote.
In light of current evidence and our results, we cannot dismiss the potential far-reaching epidemiological consequences of asymptomatic transmission of B. pertussis and an ineffective B. pertussis vaccine.17
As NVIC co-founder and president Barbara Loe Fisher commented earlier this year,
When there are a lot of people with silent asymptomatic pertussis infections, it is impossible to know who is a carrier and who is not, which means that reported cases of pertussis are just the tip of a very big iceberg. It also means that articles blaming whooping cough cases on unvaccinated or partially children are nothing more than wishful thinking and scapegoating. If vaccinated people can get silently infected and transmit infection without showing any symptoms—even after getting four to six pertussis shots—then pertussis vaccine acquired ‘herd immunity’ is an illusion and always has been.18
References:
1 Fisher BL. Pertussis Microbe Outsmarts the Vaccines as Experts Argue About Why. NVIC Newsletter Mar. 27, 2016.
2 U.S. Centers for Disease Control and Prevention. Achievements in Public Health, 1900-1999 Impact of Vaccines Universally Recommended for Children—United States, 1990-1998. Mortality and Morbidity Weekly Report 1999;48:243-8.
3 U.S. Centers for Disease Control and Prevention. Pertussis (Whooping Cough) Cases by Year (1922-2014). CDC.gov Sept. 8, 2015.
4 Broome CV, Preblud SR, Bruner B et al. Epidemiology of pertussis, Atlanta, 1977. J Pediatr 1981; 98(3): 362-267.
5 Tiwari T, Murphy TV, Moran J. Recommended Antimicrobial Agents for the Treatment and Postexposure Prophylaxis of Pertussis: 2005 Guidelines. Morbidity and Mortality Weekly Report 2005; 54(RR14): 1-16.
6 CDC. About Pertussis Outbreaks. CDC.gov Sept. 8, 2015 (updated).
7 Hinman A, Orenstein WA, Schuchat A. Vaccine Preventable Diseases, Immunization and MMWR 1961-2011. MMWR Oct. 7, 2011; 60(04): 49-57.
8 CDC. Vaccination Coverage Among Children in Kindergarten – United States, 2014-15 School Year. MMWR Aug. 28, 2015: 64(33): 897-904.
9 National Vaccine Information Center. Pertussis (Whooping Cough) & Pertussis Vaccine. NVIC.org July 5, 2016 (accessed).
10 Bisgard KM, Rhodes P, Connelly BL, et al. Pertussis Vaccine Effectiveness Among Children 6 to 59 Months of Age in the United States, 1998-2001. Pediatrics 2005;116:e285-94.
11 Witt MA, Katz PH, Witt DJ. Unexpectedly Limited Durability of Immunity Following Acellular Pertussis Vaccination in Preadolescents in a North American Outbreak. Clinical Infectious Diseases 2012;54:1730-5.
12 Misegades LK, Winter K, Harriman K. Association of Childhood Pertussis With Receipt of 5 Doses of Pertussis Vaccine by Time Since Last Vaccine Dose, California, 2010. The Journal of the American Medical Association 2012;308:2126-32.
13 Tartof SY, Lewis M, Kenyon C. Waning Immunity to Pertussis Following 5 Doses of DTaP. Pediatrics March 11, 2013.
14 CDC. Pertussis Epidemic in Washington State. CDC. gov (press release) July 19, 2012.
15 Moyer MW. The Broken Vaccine. Discover Feb. 18, 2013.
16 Warfel JM, Zimmerman LI, Merkel TJ. Acellular pertussis vaccines protect against disease but fail to prevent infection and transmission in a nonhuman primate model. Proceedings of the National Academy of Sciences 2014;111:787-92.
17 Althouse BM and Scarpino SV. Asymptomatic transmission and the resurgence of Bordetella pertussis. BioMed Central 2015;146.
18 Fisher BL. Pertussis Microbe Outsmarts the Vaccines as Experts Argue About Why. NVIC Newsletter Mar. 27, 2016.













13 Responses
Excellent article….it concerns me how many people are in denial and continue to expose the rest of us and their children to damaging effects.
Did you even read the article? 95-98% of people are already vaccinated, but people are getting sick anyway. Read the section titled “Vaccine Failure Again to Blame”. Nobody is exposing anyone to danger in this case, other than the vaccine itself.
My son is severely handicapped from the DPT vaccine! If I was able to do it again I would at leastnpay the extra for the dtap! It took me five years to prove that thae pertussis vaccine ruined my sons life!
Another source is from illegal immigrants and so-called refugees coming into our country who are carriers. The media and government will not address this as they don’t care but instead have used the increase in diseases as a call for more vaccines.
There has been an increase in tuberculosis and other transmittable diseases since this has begun. We as a Nation need to bring loud voices to the government in the hopes they will actually do something other than pass unconstitutional laws for mandatory vaccination.
Mark: The CDC reported several years ago that immigrants-illegal and those coming in legally, are vaccinated because in the countries they are leaving, Mexico for one, vaccines are mandatory. Even in South America. In fact according to some of the daily CDC reports I’ve read before the 2012 election because people were screaming how Obama was allowing too many immigrants into the country, immigrants are more vaccinated than Americans and that’s saying a lot. People need to get off of this. Outbreaks of every childhood disease in the last few years have been traced back to vaccine strains and if anything the illegals, because they are vaccinated may be infecting others.
Sadly, my daughter works in a hospital where there are three cases of meningitis infected children on her ward who were not vaccinated. She is pregnant, got the Pertussis vaccine and wants anyone near her newborn to have the vaccine. After reading this article I am confused but I want to respect my daughter’s request. She refuses to even read anything about vaccines. I have told her to get only one vaccine ( which may contain three vaccines) at a time and to spread them out as long as you can.
I totally understand where you are coming from. Three years ago, my daughter was pregnant with her fourth child. Her three children were vaccinated. She asked me to do research for her because she had been reading a lot of negative articles on vaccines. I did my due diligence and advised her NOT to vaccinate! I bought several books and gave them to my son in law to read (my daughter could not come to a conclusion). Because of fear created by the pharmaceutical companies among the mainstream media, they both decided to vaccinate their fourth child. But they spoke to their pediatrician and spread out the vaccine schedule. Yes, you have to respect your daughter’s request, but I would advise her to do her research to weigh the pros and cons. It amazes me how many people trust the medical field when so many of them (doctors and nurses) don’t know the dangers. They were taught to vaccinate and many don’t even know what is in the vaccines. It all comes down to money in the pockets of the pharmaceuticals.
Meeting of the Board of Scientific Counselors, Office of Infectious Diseases Centers for Disease Control and Prevention Tom Harkins Global Communication Center Atlanta, Georgia December 11-12, 2013.
FDA issued a warning regarding this crucial finding. Furthermore, the 2013 meeting of the Board of Scientific Counselors at the CDC revealed additional alarming data that pertussis variants (PRN negative strains) currently circulating in the USA acquired a selective advantage to infect those who are up to date for their DTap boosters (see appendix) for the CDC document Item#3), meaning that people who are up to date are more likely to be infected and thus contagious than people who are not vaccinated.
Even worse, these vaccinated asymptomatic pertussis carriers are responsible for the multiple sclerosis epidemic.
http://www.sciencedirect.com/science/article/pii/S0171298515301078
I just wonder if having pertussis primes the body to be immune to varied coughing infections. My granddaughter received the DaTP (and had a reaction, which I’m sure her busy mother did not report) but now she is subject to frequent awful coughing episodes.
It’s a candy mint, no it’s a breath mint, no it’s two mints in one! Well guess what? Vaccines are neither safe nor effective because there’s no such thing as vaccine. And there’s no such thing as immunity. But there is health by healthful living because it’s unhealthful living that causes coughing and everything else. Vaccines are always damaging because of the crap that’s in the syringe. In fact instead of being called ‘vaccines’, they should be called ‘crap in a syringe’ because that’s what they are – poisons. OK, next subject…
[url=http://buy-pillsviagra.org/]buy-pillsviagra.org.ankor[/url] priceslevitra-generic.com.ankor http://onlinewithoutprescriptionpropecia.net/
I’m so glad to see this because this is exactly what happened to me and my family. We got whooping cough from my daughters friend. They were both going to go to middle school so she got her booster shot. Mine did not get vaccinated. She had gotten the shot and came down with whooping cough a week later, I’m sure it’s no coincidence. I was the first person to get it then my two little ones my eldest children never got it nor my husband. They had their vac for it when they were young, but my little ones did not. It was so horrible for my youngest. Lasting months. We did lots of herbal remedies. Mine a month. Finally when we got over it. We got sick again for another 2month. It happened again 1 month then again and again. It was a nightmare. Then we started getting a stomach flu in between every few times. Everyone would get sick and one person would throw up. Finally a year and a half later we get a very mild version of it. Also during that winter I got diverticulitis. Then again that summer,I know it sounds crazy but I swear it’s related as all my tests were inconclusive due to not finding any of the bugs they were looking for. Well winter was coming and a friend moved in and she got a bad cough just like us it took her a month to get better. I feel we will have this the rest of our lives. Well know winter came and yes it got us again a lot less no whooping from the kids but it is very mucusy and last a long while really never clearing up now. Like living with nose allergies. Govt. Stop Using Us As A Science Expirament your making us worse spreading more disease. If vaccinated people are spreading disease what’s the point. There is non except more sickness but I’m sure that’s the point!